Vignan Yogendrakumar, Erica Tsang, Barbara Fitzgerald
ABSTRACT
Social Pediatrics, a medical sub–specialty utilizing a community–based and holistic approach to pediatric care, is increasingly recognized for its effectiveness in addressing the medical and social issues of disadvantaged populations. Exposure to social pediatrics is prevalent throughout residency, but is limited for most medical students. The purpose of this article is to describe an innovative program available to junior medical students at the University of British Columbia (UBC) for learning and practicing social pediatrics within communities of Vancouver. Through this program, medical students are trained on relevant topics, such as the importance of cultural awareness, the effects of poverty on health, and the assessment of developmental pediatric disorders. Student then participate in developmental assessments of children and assist in the formulation of management plans with families and health care teams. In the process, students gain valuable skills in developmental pediatrics, with an emphasis on collaboration and integration with school and community supports.
INTRODUCTION
Population studies have demonstrated a correlation between social and material inequities and poor health over the course of life.[1,2] Children who face financial disadvantages are prone to experiencing developmental delays and to suffering poor relationships with their community and their school. There is a need to educate incoming physicians and health care practitioners about these health inequalities, to better prepare them to address similar concerns in the future. This has led to the development of Social Pediatrics as a sub–specialty. Utilizing a complement of primary and tertiary care resources, social pediatric initiatives aim to provide a holistic, community–based approach to address the medical and social issues of disadvantaged children.[3] While exposure to social pediatrics occurs at the residency level, literature describing such exposure for medical students is sparse.[3] The purpose of this article is to introduce an innovative program at the University of British Columbia (UBC), where first– and second–year medical students learn and work in underserved communities.
The inner–city area of Vancouver, particularly the Downtown Eastside neighbourhood, ranks among the poorest in Canada.[4] Two–thirds of the children from this region start school developmentally–vulnerable.[5] In 2006, the RICHER (Responsive, Intersectoral–Interdisciplinary, Child–Community, Health, Education and Research) social pediatrics initiative was developed to provide a holistic approach to improve child health within the inner–city population of Vancouver.[4,6]
Part of the RICHER framework involves a School Developmental Pediatric Outreach Service that provides developmental assessments to inner–city school children. This outreach service has been very well–received, based on informal feedback from schools and families. However, potential areas of improvement were observed by RICHER investigators: 1) the volume of children requiring assessments vastly outnumber the available providers; 2) there are always more medical trainees who would like to learn in this setting than available positions; and 3) many children and families were unable to follow through on the long list of recommendations generated from the assessments, due to limited resources. As a result of these potential areas for improvement, UBC students and faculty developed the Global Health Initiative (GHI) Inner City Project. The project provided medical students with opportunities to learn while working with vulnerable communities and to help families and schools to meet the recommendations made during the developmental assessments. Students were also involved in recognizing the needs of children and families through formal classroom observations of behavior and through completion of developmental pediatric assessments.
The GHI Inner City Program is a two–year longitudinal program that operates on a volunteer basis. Ten first–year medical students were selected and underwent a training curriculum, designed and reviewed annually by medical students. Upon entering their second year of medical school, students were matched with children and began the formal assessment process.
Developmental Assessment
The primary element of the project is the clinical observation, assessment, and longitudinal follow–up of select children in the Vancouver School System by medical students. Armed with training in child development, observation skills, and cultural sensitivity, medical students were tasked with eliciting the histories of select children and observing them in the classroom over a series of visits. Children (ages 5-12) were identified by teachers and staff—due to concerns about developmental delay and/or behavioral abnormalities—and were referred to the supervising developmental pediatrician. After consent from the family was obtained, medical students reviewed relevant school files and elicited histories from school professionals, including teachers, counselors, youth, and family workers. A full observational assessment of the children was performed over multiple visits to the classroom and playground. By utilizing tools such as the Ages & Stages Questionnaire (ASQ), medical students assessed the children based on multiple variables, including development milestone achievement, language and communication skills, and interpersonal interactions.[7] Students often met with parents to better understand the children’s home environments and to discuss any parental concerns. Students ultimately reported their findings to the supervising developmental pediatrician, and the formal assessment was completed together with the children and their families. At the end of the assessment, the developmental pediatrician, the medical student, the school team, and the family created a follow–up and management plan. Medical students followed the children and families for one year and helped to connect them to medical services, assessments, and other community resources. In particular, medical students worked closely to facilitate recommendations with those families who have difficulty accessing health care resources. For instance, if a recommendation was made for a child to have an audiology assessment, the medical student would work with the family to ensure that it was carried out.
Curriculum
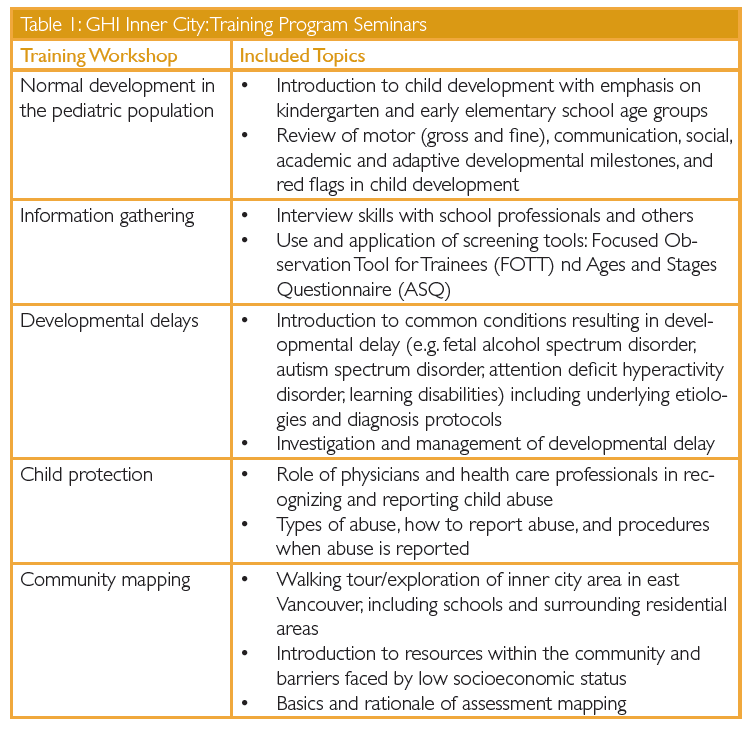
The curriculum includes training seminars, opportunities to shadow senior students during pediatric assessments, and monthly meetings to discuss cases and challenges.[Table 1] Training workshops are complemented by a manual containing useful resources that students can use throughout the year as a reference guide to assist in their respective assignments. This system is unique in that the training program was fully designed by UBC medical students. With faculty supervision, students in all four years of training came together and designed a curriculum that would satisfy their learning needs. Since its inception in 2010, the training program and curriculum have been revised on a yearly basis by the cohort of students involved in the program in that academic year. Changes to the curriculum are based primarily on student feedback, but they also take into account input from schools taking part in the program, community program leaders, and UBC faculty supervisors. The training seminars are administered by professionals from multiple disciplines, including social workers, developmental and general pediatricians, parents of special–needs children, and nurses.
OUTCOMES
Despite the growth and positive reception of the program, there are still multiple challenges. One of the primary challenges for medical students has been providing families with support to access long–term community resources. Students are involved in the developmental assessment aspect of the program for one year, and it has been difficult to maintain continuity beyond this. In order to address this challenge, medical students are asked to provide continuity of care to previous assignments in addition to performing new assessments. Medical students are provided with the results and recommendations of previous assessments to ensure that previous recommendations are met and families continue to feel supported by the program. While our cohort of medical students remains quite small in number, we hope to conduct formal surveys with both the families and the medical students to assess the impacts of the GHI program and to identify further areas for improvement.
Overall, the GHI Inner City project has grown, and it continues to develop in response to medical student and faculty interest, coupled with an unmet need in the community. From a learner’s perspective, medical students are given the opportunity to perform developmental assessments, and in the process, to learn important observational skills in child development and behavior. They also gain exposure to working with vulnerable populations, appreciate the value of integrating health care with community services and supports, and acquire first–hand experience in dealing with the social determinants of health. It would be valuable to examine whether this program impacts the medical students’ perspectives of empathy, advocacy, and social accountability. Further longitudinal follow–up would also be helpful in elucidating long–term impacts of the program, such as the students’ residency choices. From a community standpoint, the students serve as a liaison between different health care professionals to help families navigate the health care system. This grassroots initiative hopes to affect change in the lives of children living in vulnerable communities and will continue to evolve based on community need. In the coming years, formal evaluation of the program may lead to improved support for inner–city families and enhanced community partnerships.
REFERENCES
- Lloyd JE, Li L, Hertzman C. Early experiences matter: lasting effect of concentrated disadvantage on children’s language and cognitive outcomes. Health Place. 2010 Mar;16(2):371‑80.
- Stansfeld SA, Clark C, Rodgers B, Caldwell T, Power C. Repeated exposure to socioeconomic disadvantage and health selection as life course pathways to mid–life depressive and anxiety disorders. Soc Psychiatry Psychiatr Epidemiol. 2011 Jul;46(7):549‑58.
- Guyda H. Razack S, Steinmetz N. Social paediatrics. Paediatr Child Health. 2006 Dec;11(10):643‑5.
- Lynam MJ, Scott L, Loock C, Wong ST. The RICHER social pediatrics model: fostering access and reducing inequities in children’s health. Healthc Q. 2011;14:41‑6.
- Kershaw P, Trafford K, Hertzman C. Early Experiences matter: lasting effect of concentrated disadvantage on children’s language and cognitive outcomes. Health Place. 2010 Mar;16(2):371‑80.
- Lynam, M.J., Loock, C., Scott, L., Wong, S. et al (2010). Social Pediatrics Initiative. Enacting a ‘RICHER” model. A report to the British Columbia Medical Services Foundation and the Canadian Nurses Foundation. Vancouver, BC.
- Kerstjens JM, Bos AF, ten Vergert EM, de Meer G, Butcher PR, Reijneveld SA. Support for the global feasibility of the Ages and Stages Questionnaire as developmental screener. Early Hum Dev. 2009 Jul;85(7):443‑7.
Yogendrakumar V, Tsang E, Fitzgerald B. Teaching Social Pediatrics: the Global Health Initiative Inner City Project. UBCMJ. 2015: 7.1 (30-32).